Does tongue tie cause breastfeeding problems?
We don’t think there is any doubt that tongue ties cause breastfeeding problems. And the reason is that the key to successful breastfeeding is for the mother to help the baby achieve as good a latch as possible! A good latch results in pain-free breastfeeding and the baby getting good flow of milk from the breast.
A baby with a tongue tie, cannot have a good latch and cannot exercise the full range of tongue motions necessary to stimulate the breast to release breastmilk. There is now sufficient data from several studies that a tongue tie does cause breastfeeding problems. See the studies at the end of this article.
Questions that arise:
What is a tongue tie?
A tongue tie exists when the thin piece of tissue, called the frenulum, which connects the tongue to the floor of the mouth, is too thick or too tight so that the mobility of the tongue is restricted. It may affect several areas of a person’s life but has the greatest implications for breastfeeding because this is when the greatest tongue mobility is necessary for the baby to receive enough milk and for the mother to be comfortable breastfeeding and not in pain.
Are there more babies with tongue ties than 50 years ago?
It seems unlikely. Why would that be? The use of folic acid during pregnancy to prevent spina bifida has been cited as a possible cause, but there is no good evidence at all to suggest this as a cause of tongue tie.
People these days get the impression that a huge number of babies are being diagnosed with a tongue tie and wonder why tongue ties were not a problem in the past.
In general, in medicine, we are now able to diagnose more conditions than we were in the past and link them the symptoms people are experiencing. This is the case with tongue tie too. However, tongue tie is not new and it has been known for centuries that tongue ties were a problem for breastfeeding and were being corrected in primitive ways by midwives.
Additionally, many more women are breastfeeding now than say, 50 years ago, and so this issue comes to the forefront whereas before it would have been “treated” by giving the baby a bottle of formula, (and still is being “corrected” in this way, unfortunately). Problems with breastfeeding are cumulative and these days tongue ties are diagnosed in a situation when more babies and mothers are having breastfeeding problems arising from the almost universal interventions during labour and birth and interventions soon after birth, such as giving bottles of formula for low blood sugar and jaundice. Most are not getting adequate help in the hospital to prevent or treat problems early. And they are looking for solutions to their problems and they are not getting good solutions from their doctors or most other health professionals. Usually the only solution on offer is “supplement”, but many mothers don’t accept that “solution” any longer. They rightly want breastfeeding solutions to assure that breastfeeding will continue.
We have only just started, in the past 20 years, to fully recognize tongue tie as a factor in causing breastfeeding problems. And “we” unfortunately, does not include many physicians. To the point where in some hospitals, nurses and lactation consultants have been forbidden, on pain of dismissal, even to mention the possibility that the baby has a tongue tie to the parents.
Furthermore, now many more mothers don’t accept the word of doctors/midwives/lactation consultants that there is no tongue tie or that it is mild and of minimal importance. In fact, our experience is that if the tongue tie is said to be “mild” it is far more than mild and the mothers problems are far greater than minimal.

Photo 1: In this case, the doctor did diagnose a tongue tie (It is so obvious that it could be diagnosed by a 5 year old and it is indeed very tight.), but the doctor said that the tongue tie had nothing to do with the mother’s severe nipple pain, but rather was a “cosmetic problem only”. Cosmetic? What on earth could that mean? The baby has an ugly tongue?
Many health professionals also were embarrassed years ago about releasing tongue ties for “preventing speech problems”. And release of tongue tie to prevent speech problems died out when studies were published that moderate tongue ties do not mean speech problems in languages such as English whose phonemes (sounds) do not require a wide range of tongue mobility. This left many health professionals with a feeling of having been recommending a procedure that had no value. Something like the feeling they had when it was found that the virtually universal tonsillectomy and adenoidectomy in young children was being too often done without reason.
Mild tongue tie does not seem to cause problems for native speakers of English or that the “lisp” and speech impediments are minor and thus go unnoticed because of a wide variety of pronunciations of different phonemes (sounds) being tolerated by English speakers. But it does for speakers of many languages where the “r” is “rolled”, as in Spanish and many other languages, including Slavic languages and Arabic or where there are other phonemes which require a greater tongue mobility and where tolerance for “wrong pronunciation” is low and a source of ridicule.
An anecdote: When I tell parents that the baby has a tongue tie and they have never heard of this, we spend a long time explaining to the parents why the tongue tie might be a problem, what is involved in releasing it and what to do about after care (in fact we no longer recommend stretching exercises, but are starting to rethink this question also). One day, I saw a family originally from Serbia. The mother had very sore nipples. After I examined the baby, I said to the parents that the baby had a tongue tie. The father, instead of asking for a long explanation about this, immediately said “Cut it”. I was taken aback, to say the least, as the father asked for no explanation at all. When I asked him why he agreed, he said that he himself had a tongue tie when he was a child but could not roll his “r” and was mocked in school. At the age of 25 years, he finally had his tongue tie released and he could immediately roll his “r”. He did not want his baby to have the same problems as he did.
Do health professionals know how to diagnose tongue tie?
In fact, many, if not most, doctors/nurses/lactation consultants don’t know how to diagnose a tongue tie. Diagnosing a tongue tie is about more than just looking in the baby’s mouth. It is important to feel, for the “feeling” of tightness by sweeping one’s finger underneath the baby’s tongue from side to side and then trying to lift the tongue (photo 2).

Photo 2: Trying to lift the tongue makes this less obvious tongue tie more obvious. Restriction of upper mobility of the tongue suggests a significant tongue tie. Note, the lactation consultant’s right thumb is not resting on the baby’s right eye.
In photo 3 below, we see a baby with a tongue tie who does not have an obvious frenulum, never mind a tight one. But the heart shape of the baby’s tongue suggests very strongly that the baby has a restriction of upward movement of the tongue.
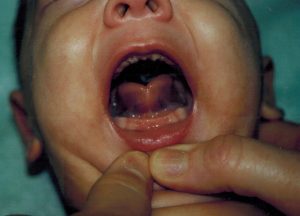
Photo 3: Tongue tie without obvious frenulum. By looking, one does not see a frenulum, so many health professionals would say “no tongue tie”.
The diagnosis of a tongue tie in the context of breastfeeding involves a combination of two elements: examination of the baby’s tongue and by observing the baby breastfeed in the context of the breastfeeding difficulties the mother and baby are encountering.
Some problems that are caused by or aggravated by a tongue tie may include:
- A baby who is not latching on
- A mother who has (early or late onset) sore nipples
- A baby who is not getting enough breastmilk from the breast
- A baby and mother who are experiencing late onset decrease in milk supply
But can’t mothers succeed at breastfeeding when their babies have tongue ties?
Of course, and many probably always did. We have seen mothers and babies at our clinic occasionally where the baby has a very tight tongue tie and yet the mother has no pain and the baby is latching on and getting plenty of milk. If the mother has an abundant supply, there may not be any problems, but then, we see many mothers with 3 and 4 month old babies who are reacting to late onset decreased milk supply (pulling at the breast, mother with late onset sore nipples, baby even not gaining, sucking his fingers much of the time, even refusing the breast). We do worry that because of the tongue tie, the mother’s milk supply will decrease with time. Also, it should be noted that many mothers believe they have “oversupply” or an “overactive letdown reflex”, but if the baby cannot handle the flow, it’s not usually because the flow is too rapid, it’s usually because the baby’s latch could be better.
Breastfeeding problems are cumulative, so that, for example, a mother who gets off to a good start with breastfeeding may have no problems in spite of the baby having a tongue tie.
But add to a baby’s tongue tie, a mother whose nipples and areolas are swollen from intravenous fluids given during labour so the baby latches on poorly or not at all, and so is given bottles and even separated from the mother etc… and now there is a problem.
Unrecognized tongue ties, however, are likely reasons for the baby failing to gain weight, for premature weaning and for early start of bottles of formula. In the past, people may have seen the symptoms of tongue ties as “the baby didn’t want to breastfeed” or “breastfeeding was too painful to bear” or “I just couldn’t breastfeed” or “the baby didn’t gain weight” or “my milk was not good enough” but may not have recognized the tongue tie as part of the cause.
Our way of releasing tongue ties
We release the tongue ties with scissors, not laser. We see many babies in our clinic whose tongue ties had been released with laser and there has been significant re-attachment. Of course, it is possible that re-attachment is less common with laser release, but then we don’t usually see those babies who have had laser release, since, presumably, things are going better. But laser release never re-attached? Definitely not true. And from what the parents say, laser release takes much longer and hurts the whole time. With scissors, the tongue tie release takes less than a second.
We do not use any anaesthetic. The best anaesthetic is breastfeeding (before the procedure and right after), and we expect the mother to stay in the room with us, or just outside by the door if she is squeamish, when we release the tongue tie. In this way, the baby can go straight to the breast and usually stops crying immediately. If the baby’s tongue and mouth have been anaesthetized, the baby cannot latch on properly or suck well and get relief and comfort from breastfeeding. The baby calming down by breastfeeding usually stops any bleeding as well. In addition, the taste of the anaesthetic by itself is probably unpleasant for the baby.
We do not recommend exercises to prevent re-attachment. We have been criticized for this, but we have seen no good evidence that they make a difference. In our experience, also, we have not seen a difference in re-attachment. For a while we were asking some parents to do the exercises and some not to. Though this was not a formal study, we saw an equal incidence of re-attachment with both groups. But there was a difference between the two groups, and that was that the re-attachment tended to be thicker and less mobile with exercises than without, where the frenulum was thinner and more mobile without exercises. And the baby and the parents hate the exercises. The exercises are painful for the baby and the parents. Nevertheless, as we constantly do about everything we do in the clinic, we are re-evaluating our position on stretching exercises.
Those who do laser release often recommend 4 to 6 weeks of exercises, several times a day. I just cannot imagine the parents doing that. Even a week later, when we see the baby and mother in followup, when I check the inside of the baby’s mouth, very gingerly, the baby cries. Babies remember and maybe still have pain.
Part 2 of the following video shows a tongue tie release (not the same baby).
Video 1: An obvious tongue tie in part 1 of this video. The pediatrician did not think the baby needed a tongue tie release because the baby was latching on and gaining weight. The fact that the mother had severe sore nipples didn’t seem reason enough to release the tongue tie.
It is important to have good lighting. And to have someone hold the baby well.
I use scissors to make a snip at 90 degrees to the edge of the frenulum and cut no more than 1 or 2 mm (no more) and then use the index finger of my left hand to push on the cut so that it opens up. When the tongue tie has been fully released, one sees only a diamond-shaped wound where the frenulum once was.

Photo 4: the appearance under the tongue after tongue tie release.
Bleeding is minimal if done this way and almost always stops as soon as the baby goes to the breast.
It is important to realize that helping mothers and babies with breastfeeding is about much more than releasing a tongue tie. Mothers need help with the ideal latching on of the baby, use of other ways of improving the breastfeeding such as breast compression and of course close follow-up. Any health professional who does tongue tie releases but does not have the skills to help the mother and babies with the actual breastfeeding should make sure that the mother does have good help and support and followup.
What are our results? (We follow all mothers and babies about 1 week after the initial release).
- When a mother has sore nipples, some mothers get immediate and long lasting pain relief.
- Some mothers get temporary relief for a few days and then the nipple soreness returns. This is very suggestive of the tongue tie re-attaching.
- Some babies have re-attachment when we see them on follow-up. However, the mother’s pain is still still gone or much improved. It seems as if the mother and baby just needed a few days to get “over the hump” and all is well. In such a case we would not re-release the tongue tie but ask the mother to watch for signs of late onset decreased milk supply.
- Increased milk supply and milk flow is sometimes very obvious, particularly when the baby is only a few days old. Once the baby is over a couple of weeks, the improvement in drinking is more difficult to document easily, but we think that it does help nevertheless to improve milk intake by the baby.
- When the mother has late onset decreased milk supply we prefer to increase the mother’s milk supply with domperidone, and then release the tongue tie a week or so later. The problem is that sometimes babies of 3 or 4 months of age will occasionally refuse the breast if the tongue tie is released before the milk supply is increased.
Your doctor/your lactation consultant/you want studies?
Here are several:
1. Geddes DT, Kent JC, McClellan HL, et al. Sucking characteristics of successfully breastfeeding infants with ankyloglossia: a case series. Acta Paediatr 2010;99:301-3
“…these results suggest that some mothers may have particular breast⁄nipple or milk ejection characteristics that contribute to successful breastfeeding of infants with ankyloglossia.”
2.Kumar M, Kalke E. Tongue-tie, breastfeeding difficulties and the role of Frenotomy. Acta Pædiatrica 2012;101:687-689
“Neonates with tongue-tie are at increased risk for breastfeeding difficulties. An early recognition of this association by primary care provider and prompt referral to a lactation consultant is important. In cases with clearly documented breastfeeding difficulties, frenotomy often results in rapid improvement in symptoms.”
3. Hall, DMB, Renfrew MJ. Tongue tie: Common problem or old wives’ tale? Arch Dis Child 2005;90;1211-1215
No abstract, a commentary.
4. Messner AH, Lalakea L, Aby J, Macmahon J, Bair E. Ankyloglossia. Incidence and associated feeding difficulties. Arch Otolaryngol Head Neck Surg. 2000;126:36-39
“Ankyloglossia, which is a relatively common finding in the newborn population, adversely affects breastfeeding in selected infants.”
5. Srinivasan A, Dobrich C, Mitnick H, Feldman P. Ankyloglossia in Breastfeeding Infants: The Effect of Frenotomy on Maternal Nipple Pain and Latch. Breastfeeding Medicine. 2006;1(4)216-224
“Timely frenotomy and breastfeeding counseling is an effective intervention, improving latch and decreasing nipple pain.”
6. Edmunds J, Miles S, Fullbrook P. Tongue tie and breastfeeding: A review of the literature. Breastfeeding Review 2011;19(1):19-26
“In Australia, initial exclusive breastfeeding rates are 80%, reducing to 14% at 6 months. One factor that contributes to early breastfeeding cessation is infant tongue-tie, a congenital abnormality occurring in 2.8-10.7% of infants in which a thickened, tightened or shortened frenulum is present. Tongue-tie is linked to breastfeeding difficulties, speech and dental problems. It may prevent the baby from taking enough breast tissue into its mouth to form a teat and the mother may experience painful, bleeding nipples and frequent feeding with poor infant weight gain; these problems may contribute to early breastfeeding cessation. This review of research literature analyses the evidence regarding tongue-tie to determine if appropriate intervention can reduce its impact on breastfeeding cessation concluding that, for most infants, frenotomy offers the best chance of improved and continued breastfeeding. Furthermore, studies have demonstrated that the procedure does not lead to complications for the infant or mother.”
7. Dollberg S, Botzerb E, Grunis E, Mimouni FB. Immediate nipple pain relief after frenotomy in breast-fed infants with ankyloglossia: a randomized, prospective study. Journal of Pediatric Surgery 2006;41,1598-1600
“Frenotomy appears to alleviate nipple pain immediately after frenotomy. We speculate that ankyloglossia plays a significant role in early breast-feeding difficulties, and that frenotomy is an effective therapy for these difficulties.”
8. Amir LH, James JP, Beatty J. Review of tongue-tie release at a tertiary maternity hospital. J Paediatr Child Health. 2005;41:243-245
“Frenotomy is a safe and easy procedure. Infants with a significant tongue-tie that is interfering with breastfeeding have shown an improvement with breastfeeding following frenotomy.”
9. Hogan M, Westcott C, Griffiths M. Randomized, controlled trial of division of tongue-tie in infants with feeding problems. J Paediatr Child Health 2005;41:246-250
“This randomized, controlled trial has clearly shown that tongue-ties can affect feeding and that division is safe, successful and improved feeding for mother and baby significantly better than intensive skilled support of a lactation consultant.”
10. Ballard JL, Auer CE, Khoury JC. Ankyloglossia: Assessment, Incidence, and Effect of Frenuloplasty on the Breastfeeding Dyad. Pediatrics 2002;110(5).
“Ankyloglossia is a relatively common finding in the newborn population and represents a significant proportion of breastfeeding problems. Poor infant latch and maternal nipple pain are frequently associated with this finding. Careful assessment of the lingual function, followed by frenuloplasty when indicated, seems to be a successful approach to the facilitation of breastfeeding in the presence of significant ankyloglossia.”
11. Geddes DT, Langton DB, Gollow I, Jacobs LA, Hartmann PE, Simmer K. Frenulotomy for Breastfeeding Infants With Ankyloglossia: Effect on Milk Removal and Sucking Mechanism as Imaged by Ultrasound. Pediatrics 2008;122;e188-e194
“Infants with ankyloglossia experiencing persistent breastfeeding difficulties showed less compression of the nipple by the tongue postfrenulotomy, which was associated with improved breastfeeding defined as better attachment, increased milk transfer, and less maternal pain. In the assessment of breastfeeding difficulties, ankyloglossia should be considered as a potential cause.”
12. Buryk M, Bloom D, Shope T. Efficacy of Neonatal Release of Ankyloglossia: A Randomized Trial. Pediatrics 2011;128;280
“We demonstrated immediate improvement in nipple pain and breastfeeding scores, despite a placebo effect on nipple pain. This should provide convincing evidence for those seeking a frenotomy for infants with signficant ankyloglossia.”
13. Garbin CP, Sakalidis VS, Chadwick LM, et al. Evidence of Improved Milk Intake After Frenotomy: A Case Report. Pediatrics 2013;132:e1413-e1417
“This case study confirms that ankyloglossia may reduce maternal milk supply and that frenotomy can improve milk removal by the infant. Milk-production measurements (24-hour) provided the evidence to confirm these findings.” (My comment: I think the authors are incorrect in adding this in the conclusions “This outcome confirms that ankyloglossia was the reason for poor milk transfer from the breast compared with the bottle rather than “nipple confusion.”)
14. McGoldrick R, Solari D, Hogan M, et al. Tongue-tie in the newborn: Follow-up in the first 6 months. Breastfeeding Review 2016; 24(3): 33-40
Conclusion. A divided TT was associated with benefits at both periods of follow-up. There was (i) an increase in overall breastfeeding rates and (ii) a decrease in maternal pain.
15. Ghaheri B, Cole M, Fausel FC, et al. Breastfeeding Improvement Following Tongue-Tie and Lip-Tie Release: A Prospective Cohort Study. Laryngoscope 2016;127(5):1217-1223
“Surgical release of tongue‐tie/lip‐tie results in significant improvement in breastfeeding outcomes. Improvements occur early (1 week postoperatively) and continue to improve through 1 month postoperatively. Improvements were demonstrated in both infants with classic anterior tongue‐tie and less obvious posterior tongue‐tie. This study identifies a previously under‐recognized patient population that may benefit from surgical intervention if abnormal breastfeeding symptoms exist.
16. Schlatter S-M, Schupp W, Otten J-E, et al. The role of tongue-tie in breastfeeding problems—A prospective observational study. Acta Paediatr 2019;108:2214-2221
“Tongue-tie had a significant impact on breastfeeding and so did low birth weights and prematurity. Frenulotomy proved helpful when breastfeeding problems were reported.”
If you need help with breastfeeding, make an appointment at our clinic.
Copyright: Jack Newman, MD, FRCPC, Andrea Polokova, 2017, 2018, 2019, 2020

