Late onset decreased milk supply
From the emails we receive and from the patients we see in our breastfeeding clinic, we believe that “late onset decreased milk supply” is a common problem and is often misdiagnosed as something else, frequently “reflux” and/or allergy to something in the mother’s milk. It’s ironic because many, if not most of the mothers who have this problem, actually started out with an abundant milk production and the milk production decreased for one reason or another. Please note that “decreased” does not mean necessarily “not enough”, only less than there was before. And this is important to understand because often the diagnosis is not considered because the baby’s weight continues to be good. Often the mother will say that her milk sprays across the room when she expresses or that she can pump large amounts of milk. But these facts do not rule out late onset decreased milk supply.
Late onset decreased milk supply may occur as early as 3 or 4 weeks after birth, but usually the symptoms may only start to become obvious around 2 to 3 months after birth.
What are the symptoms of late onset decreased milk supply?
- Obviously, in some cases, though not all, not even the majority by any means, the baby’s weight slows down or even plateaus. Some may lose weight. But, and this should be emphasized, most babies continue to gain weight, but it’s the baby’s behaviour that shows that something is not quite right.
- “Overactive letdown reflex”. If the baby cannot handle the flow, it’s not usually because the flow is too rapid, it’s usually because the baby’s latch could be better. Most of the mothers, almost every one, who have attended our breastfeeding clinic or who told me in an email that the baby’s latch was good, had babies whose latch was far from good. Many of the latches were definitely “non-functional”.
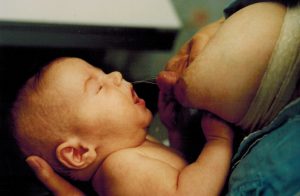
Did this baby pull away from the breast because of an “overactive letdown”. No, he pulled away because his latch was not as good as it could be. By improving the latch, including releasing the tongue tie, the baby should be able to handle the flow better. The mother is compressing the breast hoping to slow the flow but the flow is not the problem.
- Because the baby is usually still gaining weight well, the baby is diagnosed and treated with anti-reflux medications or anti-reflux formula. Neither is appropriate because the baby doesn’t have reflux. I admit that we have no proof, but we just do not believe that exclusively breastfed babies have symptomatic reflux except maybe rarely. Furthermore, anti-reflux medication like ranitidine and proton pump inhibitors are not harmless. They have been shown to cause kidney damage and increased risk of fractures, and an increase in risk of infection with Clostridium difficile, a serious gut infection. Breastmilk contains alpha lactalbumin, which, in the presence of an acidic milieu in the stomach, forms HAMLET (human alpha-lactalbumin made lethal to tumour cells) which may help to prevent cancer in children by causing tumour cells to commit suicide (apoptosis). By decreasing the acidity of the stomach these anti-reflux drugs may prevent the formation of HAMLET.

Watch this baby at the breast. For the first few minutes, the baby was drinking well. Why does this baby start to pull at the breast?
- Colic. We think the term “colic” is not accurate: Exclusively breastfed babies cry, usually, because they want more milk. This is another diagnosis that we don’t believe should be made in exclusively breastfed babies. Even if they are gaining weight well, this doesn’t mean that the baby doesn’t want more milk and as a result, the baby cries. In any case, “typical colic” does not start when the baby is 3 months old or older.
- On the other hand, the parents may state that their baby is not fussy or upset a lot of the time. It is often true that the baby is not fussy when not on the breast, but the baby spends a lot of time sucking his hand or his fingers, and thus is generally content. But the baby spending long periods sucking his fingers is not normal, though many parents (and pediatricians) believe it is. It is not and spending long periods of time sucking his fingers is a sign of late onset decreased milk supply.
- Allergy to something in the mother’s milk. This is usually felt to be a reaction to cow milk protein, usually, or soy protein or innumerable other proteins in the mother’s milk. But again, without definite proof, I am not convinced that this occurs in exclusively breastfed babies except very occasionally. Indeed, small amounts of cow milk protein and other “accused” proteins, such as peanut protein, are there to decrease the risk of allergic reaction in the baby and most recent evidence suggests that exposing babies to possible antigens (such as cow’s milk protein) can actually decrease the risk of allergy. Even blood in the baby’s bowel movements does not prove that the baby is allergic to something in the milk (see below).
- So why the blood? We have a hypothesis, but we don’t know for sure. I think this is the one place where low fat, high fat milk actually may play a role. If the milk supply decreases and the baby pulls away from the breast when the flow slows, the baby drinks mostly low fat milk. The stomach empties rapidly, along with the acid and other enzymes which normally would not enter the intestines and the fluid will move rapidly through the intestines to the large intestines and will cause irritation of the lining of the gut and bleeding. The endoscopy done by the pediatric gastroenterologist will show inflammation, and the diagnosis will be “confirmed”; allergic colitis. Really? NO!
An illustrative case report of how late onset decreased milk supply can cause blood in the bowel movements.
Here is a what happened to one mother whose baby was diagnosed with allergy to breastmilk because the baby was having blood in the bowel movements.
My baby had blood in stool a few months ago. The physician suspected milk protein allergy and had me eliminate dairy from my diet. You wrote me back that it was more likely late onset decreased milk supply. I was started on domperidone 90 mg daily. My milk supply dropped again, so the dose of domperidone was increased to 120 mg (12 pills) daily and we saw lactation consultant. She diagnosed tongue tie causing shallow latch. Tongue tie was released by a pediatrician one month later. At this point things were now perfect. I started dairy products again three weeks ago. I decreased the dose of domperidone from 120 mg/day to 40 mg daily by 10 mg every 3 days (my comment: this is way too rapidly. We recommend decreasing the dose by 10 mg a week, so that if the mother was taking 120 mg, she would take 110 mg for a week, then 100 mg for a week and so on). Milk supply dropped. Two days later blood in stool again and off and on for 3 days now. I upped my domperidone to 90 mg daily again.
My baby had milk proteins for 3 weeks and no blood. Is it safe to assume not allergy causing bloody stool? (my comment: I never thought it was allergy to something in the milk).
- See also the next point. Typically, the baby will pull at the breast, cry at the breast, release the breast and latch on again, pulling again and releasing the breast again. The baby may even refuse to take the breast completely, though most continue to breastfeed during the night.
- “Nursing strikes”. This was a common diagnosis made amongst many exclusively breastfed babies or older babies who refuse to breastfeed even though they never received any bottles and were growing well and gaining well for a while. This “nursing strike” tends to occur in babies of 4 or more months old. But the babies usually breastfeed well during the night. The baby feeding well during the night but almost not at all in the day is typical of late onset decreased milk supply.
- The mother may develop “late onset sore nipples”. Why should this happen? When milk flow slows, the baby may slip down on the nipple instead of maintaining a deep latch, the baby may “bite”, as the mothers say, and also the baby pulling at the breast without letting go can certainly cause the nipples to get sore. Mothers will often say that “they, the mother, had become lazy” in how they latched the baby on, but there is no reason to help a 4 month old latch on. The baby does it all on his own.
- Breastfeedings may be very long, or, more commonly, very short, the baby pulling away from the breast when the flow of milk slows down. When the feedings are very short, the baby may start sucking his hand or fingers much of the time. This is not normal for the baby to suck his hand or fingers much of the time, though we used to say it was.
- A baby who was sleeping through the night, may start to wake up again frequently. On the other hand, a baby who was waking up to feed during the night may start to sleep through the night, perhaps to the delight of the parents, but this may not be a good sign.
- The baby is “self-weaning”. Babies under the age of 3 or so do not “self-wean”. “Self-weaning” is thought to be the case because of the baby refusing the breast.
- In the older baby, one may see a baby not gaining weight and yet refusing to eat solids. This is taken as proof by many pediatricians and nutritionists that there “is nothing in breastmilk after the first few months”. But they can only say this because they do not watch the baby on the breast, and even if they did, they would not know what to watch for. So, triumphantly, the mother is told that the baby is using too much energy sucking all day long and getting no calories. But why would the baby refuse solids if he’s gaining little weigh? It is true that the baby is not getting a lot of nutrients and calories, but not because there is nothing in breastmilk after the first few months but rather because the baby is not getting much milk at all. And this makes the baby ketotic, just like someone on some diets that try to induce ketosis in the dieter. When you are ketotic, you lose your appetite. So the baby has no interest in eating solids but continues on the breast because he gets comfort and security from the breast.
When does the decrease in milk supply and flow begin?
We think it begins much earlier than the mothers suspect. Babies who were doing well, start to be a little fussy, often explained by “he’s getting older, more aware of the world”, that sort of explanation. Or the babies are sucking their fingers and this is explained away as “normal” for age. But then at some point the parents can’t ignore or explain away what’s happening. We are sure that these mothers have had a long period, several weeks, of decreasing milk supply and flow and that when it becomes critical, they recognize there is a problem, but think it’s sudden onset. At this point the baby is diagnosed with either “reflux” or “allergy to something in the mother’s milk”, neither of which is correct. Unfortunately, if the baby is switched to formula, any formula, not necessarily “hypoallergenic” formula, the baby gets better. Why? Because he was truly allergic to something in the breastmilk? No!! This proves nothing. The real reason? The baby now drinks more milk.
Why would the mother have a decrease in her milk supply?
• Often the baby’s latch is not as good as it could be. The mother may or may not have sore nipples because of the less than good latch but often she overcomes the sore nipples because the baby receives good flow at the breast. These are the mothers who were told years ago “It’s normal to have sore nipples but you won’t have any more pain after three weeks”. Years ago? When I first started the breastfeeding clinic, mothers were almost universally told this from what I could ascertain, at least from what the mothers coming to the clinic were telling me.
And why would the baby’s latch not be as good as it could be? Because of 1. How the baby goes to the breast and positioning and latching the baby on the breast 2. Use of artificial nipples such as bottles and nipple shields and more than occasional use of pacifiers (A baby who is really breastfeeding well should not need a pacifier, and the introduction of the pacifier may be an early sign of late onset decreased milk supply. And as a result of the use of the pacifier the milk supply decreases even more) 3. The baby has a tongue tie. Some tongue ties are obvious, but many tongue ties are more subtle and require an evaluation that goes farther than just looking, but includes feeling under the baby’s tongue as well and knowing what to feel for. Unfortunately, few health professionals, including lactation consultants, know how to evaluate whether or not the baby has a tongue tie. Even if a tongue tie is released, it is often only partially released and/or has re-attached. 4. The mother has had a decrease in her milk supply. Late onset decreased milk supply is common. And when the milk flow slows, the baby tends to slip down on the nipple and the latch is even worse, so that decreased milk supply itself can lead to more decrease. And click these links Really good drinking with English text, Twelve day old nibbling, English Text, “Borderline” drinking for video clips showing babies drinking well at the breast, or not. Watch the videos, read the texts and then watch the videos again. Following the Protocol manage Breastmilk intake may change things so he does gain well.
• The mother has been feeding the baby on one breast at each feeding, without offering the other breast. It used to be usual, when mothers were breastfeeding, to automatically offer the other breast as the baby started to fall asleep on the first breast. In the past few years, mothers have been advised to feed the baby on just one breast at a feeding, even to offer the same breast only for several feedings at a time (“block feeding”). But if the baby is not drinking (see the videos mentioned in the previous paragraph), the baby is not getting the hindmilk because the baby is not getting any milk. And the result of feeding on just one side to follow a rule? A decrease in the milk supply.
• The mother has started the birth control pill, an IUD with progesterone or another type of birth control which is hormone based. These methods undoubtedly cause a decrease in the milk supply in some or even many nursing mothers. Mothers are usually told that these hormonal methods of birth control do not affect the milk supply. They are told wrong. Some mothers say they do not get a change in their milk supply while on hormonal methods of birth control. Perhaps, not all people react in the same way to all medications.
• It is well known that a new pregnancy will decrease the milk supply. In the exclusively breastfeeding mother whose baby is not receiving bottles, a pacifier or where the mother is not holding off on feedings and the mother has not yet had her period, the chance of pregnancy in the first six months is very low, about the same as with a birth control pill. Many babies will continue breastfeeding even if the milk supply is considerably decreased because they are breastfeeding for more than the milk, but rather for the comfort and security of breastfeeding. Other babies, for whom the milk flow is important, will fuss at the breast and many will stop breastfeeding, especially if given bottles.
• Some medications may decrease the milk supply. It is obvious that bromocriptine (Parlodel) and cabergoline (Dostinex) should not be used in breastfeeding mothers. The two drugs are supposed to turn off milk supply. But imagine that in Eastern Europe and in Greece and probably some other countries they are used to prevent postpartum engorgement (the treatment for postpartum engorgement is to prevent it by getting the baby breastfeeding well) and for mastitis (no words can describe how ridiculous this approach to treating mastitis is). Oral antihistamines, especially the older ones, also decrease the milk supply, based on multiple reports from breastfeeding mothers, though there is no study that ever showed this. It is possible that pseudoephedrine can also decrease the milk supply. Both antihistamines and pseudoephedrine can be found in over the counter cold and allergy medicines. Bupropion (Wellbutrin) an antidepressant unlike most other antidepressants may decrease the milk supply, but we don’t know for sure.
• Can postpartum depression, exhaustion, mother’s diet affect milk supply? Everyone seems to believe it, and it could very well be true, I don’t know, but there is no good evidence for these factors.
So, what can be done to prevent and to treat this problem?
It is always best to prevent problems than to treat them, or perhaps better said, the best treatment of any problem is prevention. And what does that imply? Get the best latch as soon as possible after the baby is born. If the mother has painful nipples, then the baby’s latch is not good no matter how it looks from the outside. In the first few days and even later, a good latch and breast compression are useful ways of getting more milk into the baby and helps prevent frustration and early introduction of bottles or nipple shields which result in decreased milk getting to the baby from the breast. Skin to skin contact is also very important to the initiation of breastfeeding. The earlier breastfeeding problems are addressed, the easier they are to treat.
When we ask our patients whose baby has a very significant tongue tie whether the hospital staff checked the baby for tongue tie, the answer is most frequently “no they didn’t even look”. Next most frequent answer is that they said there might be a tongue tie but it’s not significant. These tongue ties, when we see the mother and baby, are obviously very significant. And finally, the answer is often also, there is no tongue tie.
And what else?
• It is not a good idea to feed the baby on just one side, to follow a rule. Yes, making sure the baby “finishes” the first side before offering the second can help treat poor weight gain or fussiness in the baby, but rules and breastfeeding do not go together well. If the baby is not drinking, actually getting milk, there is no point in just keeping the baby sucking without getting much milk for long periods of time. The mother should “finish” one side and then offer the other. The approach of feeding one side without “listening” to the baby ends up with a decrease in milk supply.
Furthermore, babies tend to get less milk in the late afternoon than in the morning, so what might work in the early morning may not work in the early evening. If the baby cries and fusses in the evening, mothers who has been advised “one breast/feeding” may keep putting the baby back to the same breast and finally conclude that she needs to give the baby a bottle of formula. And as the milk supply continues to decrease, the problem may get worse and worse. Even if the mother puts previously expressed milk into the evening bottle, this is not the answer to the problem. The bottle only makes the problem worse.
On top of that, what may work when the baby is a month old, say, may not work when the baby is 3 or 4 months, yet, believing that one breast/feeding is the way to go, the milk supply continues to decrease and many symptoms of late onset decreased milk supply may occur.
• Medications that decrease milk supply should be avoided. These are discussed above. It is almost always possible to avoid oral antihistamines. For seasonal allergies, local treatment is preferable, not only to prevent decreased milk supply. Why give the whole body a drug when it is only the eyes or nose that needs treatment? There are nasal and eye drops which can be used, and inhalers for respiratory symptoms. The use of cabergoline (Dostinex) and bromocriptine (Parlodel) is contraindicated in breastfeeding mothers because they may turn off the milk supply.
• Early intervention for breastfeeding problems is important. Problems that are difficult to treat when the baby is 8 weeks old, could have been easy to treat when the baby is 8 days old.
If the problem of late onset decreased milk supply already exists?
First and foremost, eliminate whatever medications the mother is taking that might decrease her milk supply.
If the mother is feeding one breast at a feeding, she should start offering both breasts at each feeding.
It’s not too late to release a tongue tie.
If the baby is four months of age or older, food can and should be started rather than formula, especially by bottle, though if the baby will take the lactation aid at the breast, then formula is an option. So is donated breastmilk. But a bottle interferes with breastfeeding and in the context of a decrease in milk supply, may result in the baby refusing the breast altogether. And how much of the solids should be given? As much as the baby will take, as frequently as the baby will take them without forcing. Commercial infant cereals, though beloved by pediatricians, are low in nutrients, except iron, most of which ends up in the baby’s diaper. They taste, at best, blah, are often constipating. There is nothing magical about them. For more information on Starting solids,
But it’s even more important to increase the milk supply than to give food. Domperidone can increase the milk supply and milk flow. We start with 30 mg (3 tablets) 3 times a day and sometimes go up from there in two steps, first to 40 mg (4 tablets) 3 times a day and then 40 mg (4 tablets) 4 times a day, or 50 mg (5 tablets) 3 times a day (for convenience). Click this link for information on domperidone.
Need breastfeeding help? Make an appointment at the International Breastfeeding Centre.
Copyright: Jack Newman, MD, FRCPC, Andrea Polokova, 2017, 2018, 2020

