Is My Baby Getting Enough Milk? (Part 2)
Our approach to increasing the baby’s intake of breastmilk when the baby is not getting as much as we would like is based on four principles:
1. When breastfeeding goes well it is easy and pleasant for the mother and the baby. When breastfeeding is not going well, it should be as easy and as pleasant for the mother and baby as is possible given the circumstances.
2. First and foremost, we attempt to correct the difficulties without jumping to supplementation and bottles.
3. Breastfeeding is much more than breastmilk. Breastfeeding is a close, physical and emotional relationship between two people who are usually in love with each other.
4. It is possible to breastfeed even if the baby needs to be supplemented.
Thus, when breastfeeding is not going well, what does this mean in terms of our approach?
1. This means that as long as the baby is latching on reasonably well on the breast, that we do not encourage the mother to express or pump her milk as a way to increase milk supply. Pumping and hand expression are work, time consuming work, and we believe that when a mother feels obliged to pump or express her milk, she is likely to stop breastfeeding much earlier than if she does not pump or express her milk. Or she is much more likely to go to exclusive pumping and bottle feeding.
There is plenty of evidence that what a mother can express, or pump is not the same as what the baby receives from the breast. A baby who is well latched on can get much more than what a mother might be able to pump. A baby poorly latched on will get less milk. Thus, in case the mother is told to pump in order to increase her milk supply and she gets very little milk, she might be discouraged and think that her baby also gets very little from the breast and give up breastfeeding altogether.
On the other hand, if the mother is able to express all the milk the baby needs, she should have been able to feed the baby exclusively at the breast and therefore the approach should be not to just say, “That’s fine, wonderful”, but help her so that the baby can get the milk from the breast.
Breast compression is like pumping but instead of pumping into a container, the mother pumps directly into the baby, eliminating the “middle man”.
2. This means that the mother and baby should first get help with breastfeeding (improve the latch, use breast compression, switch sides), and when a baby truly needs supplementation, the supplement should be given at the breast with a lactation aid at the breast. Because:
- Breastfeeding is more than the milk and even if the mother is supplementing the baby with formula, supplementing the baby at the breast means the mother and baby are still breastfeeding
- Babies learn to breastfeed by breastfeeding
- Mothers learn to breastfeed by breastfeeding
- The baby continues to get milk from the breast even as he is being supplemented
- With supplementation at the breast, the milk supply increases
- The baby is much less likely to reject the breast, refuse to latch on, in other words, than if he is supplemented by bottle. In fact, he will not reject the breast if the lactation aid is used properly with the baby having as good a latch as possible and the tube properly placed. Other methods, such supplementing with an open cup or finger feeding, though better than a bottle are still not methods where the baby is being supplemented on the breast.

Photo 1: A baby being supplemented at the breast with a lactation aid. This method teaches a baby how to breastfeed, teaches the mother how to breastfeed, prevents breast rejection by the baby, allows the baby to continue getting milk from the breast even while being supplemented. This method also preserves breastfeeding which is much more than breastmilk.
The baby is not getting enough milk from the breast! What do we do now?
1.First of all, we help the mother and baby achieve the best latch possible. The better the latch, the more milk the baby will receive from the breast. Look at this baby at the breast (photo 2). The latch is “asymmetric”. Why is it better?

Photo 2: This baby has an asymmetric latch,
– the chin is in breast, but the nose is not. He covers more of the areola with his lower lip than his upper lip and thus more of the breast is above/over the baby’s lower jaw. All of us who discuss breastfeeding, emphasize the importance of getting more of the breast into the baby’s mouth. And an asymmetric latch gets more of the breast into the baby’s mouth, at least more of the breast where the baby’s lower jaw is. The baby is thus able to stimulate better the release of milk from the breast because of the sucking movements of the lower jaw. Compare with this baby’s latch (photo under this paragraph, photo 3):
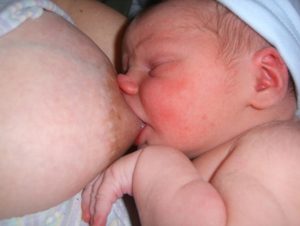
Photo 3: This baby has a poor latch – the opposite of an asymmetric latch, the nose is in the breast, the chin is not. There is more breast under the baby’s upper lip than above the lower lip. The maxilla (upper jaw) does not move and thus does not stimulate the breast well to release milk from the breast.
2. Once the mother has the baby latched on as well as possible, we show her how to know the baby is getting milk. How do we know the baby is getting milk? See video 1 below.
Video 1: This baby is drinking very well at the breast. The pause as he opens his mouth to the maximum is a sign that his mouth is filling with milk. The longer the pause, the more milk the baby received. As long as the baby is drinking like this, there is no need to use breast compression, or take the baby off the breast or offer the other breast.
Video 2: This baby is hardly drinking at all. There are no pauses at all in the chin. The baby is getting almost no milk.
It is for this reason “just feed the baby on one breast at each feeding” or “do block feeding” so the baby gets more high fat milk is so likely to cause late onset decreased milk supply . If a baby is not drinking at the breast, the baby is not getting high fat milk. He’s getting no milk. And persistent feeding on just one breast at a feeding will inevitably lead to a decrease in milk supply and milk flow to the baby.
3. Thus, when the baby is not drinking very much at the breast any longer, we recommend the mother start breast compressions See video 3.
Video 3: Breast compressions. When a baby is sucking but not drinking much, the mother starts to compress her breast, with the result that the baby gets more milk. The mother compresses the breast and maintains the compression steady as long as the baby drinks. She then releases the compression. She waits to see if the baby starts to drink again. If he sucks but does not drink, she repeats the compression, and so on until the baby hardly drinks.
4. When breast compressions no longer seem to get the baby more milk, the mother should offer the baby the other breast and repeat steps 1 to 3. If the baby is not getting enough milk, he should be happy to take the second side. The problem is that many mothers will keep the baby on the one breast until the baby is fast asleep. If he is fast asleep, he may not wake up to take the second side even if he would take more milk.
The next two steps depend on the clinical situation. Neither may be necessary, and in fact for the baby in this video, neither was necessary. Steps 1 to 4 were followed, and the baby started gaining weight without any galactogogues or supplementation used. He just got more and more milk as the mother’s milk supply increased with a better latch and breast compressions.
Video 4: A baby showing “borderline drinking”. There may not be enough drinking for the baby to gain weight well, but the baby is drinking enough so that the baby will not get ill or into trouble. In fact the baby did very well without galactogogues or supplementation.
On the other hand, in some cases supplementation, discussed already, will still be necessary and if so should be given on the second breast after the baby is no longer receiving much milk on that side, but again, before the baby is too sleepy. If the baby is very sleepy, inserting the lactation aid may result in his slipping off the breast.
Video 5: Inserting a lactation aid. Babies respond to milk flow. When the flow slows, the baby tends to fall asleep at the breast. When flow is increased, in this case with a lactation aid at the breast, the baby wakes up and sucks vigorously.
And/or domperidone should be prescribed for the mother.
5. In some cases, starting the mother on domperidone may be enough, along with steps 1. To 4. We start with 30 mg (3 ten mg tablets) 3 times a day and sometimes go up from there in two steps, first to 40 mg (4 tablets) 3 times a day and then 40 mg (4 tablets) 4 times a day, or 6 tablets, 5 tablets, 5 tablets (total 16 tables) for convenience. One 10 mg tablet 3 times a day as many physicians prescribe is actually rather useless. What’s the point of prescribing a useless dose of a medication?
For those frightened of domperidone, let me say that it is one of the safer medications around. The warning (in January 2015) by Health Canada is not based on good evidence and there is no good evidence there is a risk for any cardiac side effect with domperidone. (In fact, it is not a Health Canada warning, but rather an endorsed warning which originates from a company that makes domperidone). It is bizarre that the fax sent out by Health Canada in January 2015 does not mention any references though apparently this is not rare for Health Canada.
The warning is a word for word repetition of the statement by the European Medications Agency which gets many of its ideas from the drug manufacturers and formula companies. In spite of several deaths in Europe in mothers taking the birth control pill (and in Canada too – 23 deaths in 8 years in Canada as reported by Health Canada), everyone says that the birth control pill is worth the risk. Well, considering there are methods of contraception other than the birth control pill I would dispute that. But of course, the birth control pill is very much popular with physicians and other health professionals and pharmaceutical companies make a lot of money on the birth control pill, which is not the case with domperidone.
We checked with Health Canada in 2012 when all this hullabaloo started about domperidone in Canada. Health Canada has neverreceived a report of a death in a breastfeeding woman taking domperidone. We checked again after the January 2015 warning. No reports of any deaths attributable to domperidone in the age group of mothers breastfeeding. In fact, they have not had any reports of any significant side effects that can definitely be attributed to domperidone in patients of any age. Furthermore, I personally have treated tens of thousands of mothers with domperidone in much larger doses than Health Canada’s recommended maximum dose and have recommended it for many more who then received a prescription from their own family doctor. Very few mothers had any side effects at all and those who did had very minor, transient ones that disappeared within days.
How long do we recommend domperidone?
We now encourage mothers to keep taking the domperidone until the baby is well established on solids. That way, if the milk supply decreases when the mother decreases the dose of domperidone, the baby can make up the extra calories and nutrients he needs by eating more food until the mother can bump up the domperidone again. See the website information sheets on domperidone including the one on stopping domperidone. See also the next chapter. We generally recommend dropping 1 pill per day a week, always on the same day of the week, so if the mother is taking 12 pills a day now, she will take 11 pills a day for a week, then one week later 10 pills etc.
In some cases, it is not necessary to keep taking the domperidone. For example, we often use domperidone for a mother whose baby is not latching on. Even if the mother is expressing all the milk the baby needs, we believe that more milk means faster flow and faster flow means the baby is more likely to latch on. Once the baby is latched on, our experience shows that she no longer needs domperidone as the baby will get the milk and increase the flow when he is latched on well. In this situation, the mother can wean off the domperidone more quickly and before the baby is taking solids.
What about the side effects we hear about when stopping domperidone?
Although very few of our own patients have ever complained of significant side effects when stopping domperidone slowly as we recommend, there are discussions on the internet about depression, sleeplessness and anxiety associated with stopping domperidone, almost always when it is stopped too quickly. So stopping slowly, one pill a week (see above) is better than stopping quickly.
Need help with breastfeeding? Make an appointment with our clinic
Copyright: Jack Newman MD, FRCPC, Andrea Polokova 2017, 2018, 2021

