母乳喂养预防婴儿低血糖 (Low Blood Sugar)
There are two measures that should be introduced in hospital practices after birth and whose absence is causing many mothers to stop breastfeeding even though they had originally intended to breastfeed.
婴儿出生后,有两项应该被纳入但医院并没有的临床实践措施。因为缺乏这两项措施导致许多原本打算母乳喂养的母亲停止了母乳喂养她们的宝宝。
First, babies should be skin to skin with their mothers immediately after birth. It is proven that a baby who is skin to skin with his mother maintains blood sugar levels better than a baby who is not or who is in an incubator. Skin to skin contact, without the baby being dressed obviously, should be routine postpartum care for the first few hours after birth. Not only does the baby maintain his blood sugar better, but also, is much more stable with regard to his heart rate, respiratory rate and blood pressure.
第一项措施是当宝宝一出生就应该立刻和母亲进行肌肤接触。实验已经证实一个和母亲进行过产后肌肤接触的宝宝会比没有进行肌肤接触或在恒温箱里的宝宝能够维持正常血糖值。医院在初生儿前几个小时内的例行产后照謢,应该减少不必要的衣物,与母亲尽量完全肌肤接触,这样不只是更佳维持婴儿血糖正常值,同时更可以保持宝宝心跳及呼吸速率和血压稳定。
As well, skin to skin contact after birth provides an opportunity for babies to start breastfeeding and getting breastmilk from the breast soon after birth. Breastmilk is another way to help maintain blood sugar levels in the baby, much better than formula.
此外,产后肌肤接触提供了一个好时机,可以在出生后马上开始母乳喂养,婴儿从乳房可以吸到乳汁。母乳比配方奶更能帮助宝宝维持正常血糖值。
Secondly, mothers should be shown how to know whether their baby is getting breastmilk from the breast – that is to be able to tell whether the baby is drinking well or not. If the baby is drinking well, the mother should be re-assured; if the baby is not drinking well, then the first step to take is to improve the breastfeeding and help the baby get more milk from the breast.
第二项措施是教妈妈们分辨她们的宝宝是否从乳房吸到了奶—也就是说,妈妈能够知道宝宝吸奶吸得好还是不好。如果宝宝吸得好,妈妈应该被鼓励肯定; 如果吸得不好,那么首先需要做的是改善母乳喂养,并且帮助宝宝从乳房得到更多乳汁。
Hypoglycemia (low blood sugar) is one of the commonest reasons for formula supplementation in the first few days after birth. But most babies are tested for low blood sugar for no good reason, and most babies get formula by bottle also unnecessarily.
在宝宝出生后头几天需要补充配方奶的最常见的理由之一就是低血糖症。但是大多数婴儿在没有充分的检视下就被判定为低血糖,而且大多数婴儿是没必要用奶瓶来补充配方奶的。
- Doing routine blood sugars on every baby at birth is another example of how “worrying about being sued” causes damage to babies and creates unnecessary anxiety in the parents and results in unnecessary “treatment”. But many hospitals in the US have this policy and more and more in Canada. Interestingly, most pediatricians and neonatologists don’t seem to know what normal is. They look at a number and say “give formula”.
- 出生后为宝宝做例行的血糖监测是另一个“担心被起诉”的例子, 因此造成婴儿损害和父母产生不必要的担心,并最终导致了本来不需要的“治疗”。但是,在美国很多医院有给新生儿做例行血糖监测的规定,在加拿大越来越多的医院也这么做。 有趣的是,大多数儿科医生和新生儿专家们似乎都不知道什么是正常的血糖。他们看到一个血糖值,然后就建议“加配方奶”。
- In fact, nobody agrees on what is a normal blood sugar in newborns. Everyone has a different number they consider “too low”.
- 事实上,目前对于新生儿血糖正常值并没有达成共识。每个人认为的血糖“过低”的数值都不一样。
- The blood sugar in babies is more or less the same as the mother’s blood sugar at birth and then over the next 1 to 2 hours the sugar drops, for some babies, into the range many would call “too low”. But this drop in the blood sugar is NORMAL! (see the graph). And the blood sugar rises again over the following hour or two even if the baby is not fed. This has been shown not only in humans but also in all mammals that have been studied. Treating “low blood sugar” in this circumstance is treating NORMAL and thousands of babies across North America are being unnecessarily supplemented with formula for what is a normal blood sugar.
- 刚出生时,宝宝和母亲的血糖值大约相同,然后在接下来的1到2个小时内宝宝的血糖会下降。其中一些宝宝的血糖会下降到所谓的“过低”的范围内。但是,这种血糖值的下降是正常的!(见下图)。即使不给宝宝喂食,血糖也会在随后的一两个小时内再次升高。这不仅体现在人类身上,在所有已经被研究过的哺乳动物身上都表现出来了。在这种情况下实际上是对正常婴儿治疗“低血糖”。在北美地区,数千名宝宝正在因为正常的血糖值而添加了其实并不需要的配方奶。
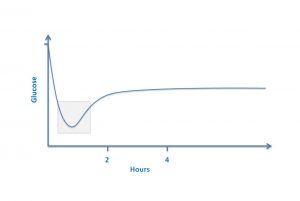
Normal glucose levels in normal newborns in the first hours after birth
一般新生儿出生后在最初几个小时内正常的血糖变化
(横轴:小时;纵轴:血糖值)
- Skin to skin contact with the mother maintains a higher blood sugar in the baby than separation of the mother and baby. Skin to skin contact also affords the baby an opportunity to feed at the breast.
- 和母婴分离的情况相比,婴儿与母亲进行肌肤接触有助于宝宝维持较高的血糖。产后肌肤接触也为宝宝提供了一个成功在乳房上吸奶的良好时机。
- The mother’s colostrum is the best milk and bank breastmilk the second best to prevent and treat low blood sugar in newborn babies. This is because breastmilk does not stimulate the production of insulin in the baby, as does formula. For this reason, we recommend that mothers whose babies are at high risk for low blood sugar express and store their milk starting at 35 to 36 weeks gestation so the baby, if necessary, can get colostrum instead of formula. There is no evidence that hand expression of milk at this stage increases the risk of premature birth. See the photo that shows the amount of colostrum one mother expressed before the baby was born.
- 母亲的初乳是提供最佳预防和治疗新生儿低血糖的食物,其次是母乳库的人乳。这是因为人乳不会如同配方奶一样会刺激宝宝体内产生胰岛素。因此,我们建议,如果婴儿患低血糖症的风险比较高,母亲从孕期35到36周开始可以把自己的乳汁挤出储存起来。这样在需要补充的时候,婴儿可以吃到初乳而不是配方奶。并无证据显示在这个时期用手挤出乳汁会增加早产的风险。下面的图片呈现了一个妈妈在婴儿出生以前挤出并储存起来的初乳数量。

Prenatally expressed colostrum in a diabetic mother
一个妈妈在产前挤出的初乳
- There is evidence that babies who are at risk for low blood sugar and are fed at the breast immediately after birth are less likely to become clinically hypoglycemic and actually have higher blood sugars than babies fed formula as their first feeding.
- 已有实验证明,对于具有低血糖风险的宝宝,只要在出生后立即进行母乳喂养,就比较不会出现临床低血糖症。实际上,和用配方奶进行第一次喂养的婴儿相比,立即进行母乳喂养的宝宝可以维持较高的血糖值。
- There is no evidence that a baby who is born big (some hospital policies say 4 kg=8lb 12oz or higher) is at risk for low blood sugar if his mother is not diabetic. On the contrary, such babies are at lower risk of hypoglycemia because they have lots of body fat that can be broken down into compounds called ketone bodies.
- 没有实验证明在母亲没有糖尿病的情况下,出生时的巨婴(一些医院是指出生体重≥ 4公斤的婴儿)有低血糖的风险。相反的,这些婴儿的低血糖风险更低,因为他们体内有大量的脂肪可以分解成一种被称为酮体的化合物。
- Ketone bodies protect the baby’s brain from the effects of low blood sugar and ketone bodies are present in much higher concentrations in the blood of babies breastfed (or fed colostrum or breastmilk) than in the blood of babies formula fed. Babies fed both breastmilk and formula have a lower but intermediate response.
- 酮体保护宝宝的大脑免受低血糖的影响,酮体在母乳喂养(用初乳或人乳喂食)的宝宝血液中的浓度远高于配方奶喂养的宝宝。而母乳和配方奶混合喂养的宝宝酮体含量较低而介于两者之间。
- There is no need for a baby at risk for low blood sugar (infants of diabetic mothers, both type 1 and type 2) to automatically go to special care. They should stay with the mother, skin to skin, be fed on demand and get help from the nursing staff to make sure the baby feeds well at the breast. Pre-expressed colostrum can be fed by spoon, syringe or lactation aid at the breast.
- 对具有低血糖风险的婴儿(I型和II型糖尿病母亲的宝宝)没有必要给予特殊护理。他们应该和母亲在一起,进行肌肤接触和按需喂养,并且得到护理团队的帮助以确保宝宝在乳房上正确含乳充分进食。那些预先挤出的初乳可以用汤匙、注射器,或哺乳辅助器在乳房添加。
- Bottom line? There is a lot of hysteroglycemia out there and the “treatment” of it is causing many babies to be unnecessarily supplemented with formula often with bottles. In one case of a mother who contacted me, the baby was admitted to the NICU because an unnecessary blood sugar was done shortly after birth (during the time that the blood sugar sometimes NORMALLY drops to “hypoglycemic” levels.) The baby had an intravenous was given formula. The mother was feeding with a nipple shield (for reasons that did not seem clear, probably because the baby refused the breast after receiving bottles, but to me NO reason for nipple shield use is clear) and pumping her breasts. The baby was in the NICU for several days at great cost to the health system. All because of an unnecessary blood sugar being done as a “routine”. This baby had no risk factors for hypoglycemia.
- 什么是医疗底线呢?世界上有不少医疗人员患有“血糖恐惧症”(是指医疗人员过度担心宝宝血糖因而造成不必要的检测),而对血糖的 “治疗”导致很多宝宝在不必要的情况下用奶瓶添加了配方奶。有一个妈妈曾经与我联系,她的宝宝被送进了新生儿加护病房,原因是宝宝在出生后不久接受了不必要的血糖测试(在刚出生时会正常下降到“低血糖”值时)。宝宝接受了静脉注射治疗,也添加了配方奶。妈妈在哺乳时用了乳头保护罩(这样做的原因似乎不太清楚,可能是因为宝宝在用奶瓶喂养后拒绝吃妈妈的乳房。但我觉得没有理由使用乳头保护罩),也使用吸奶器集乳。这个宝宝在新生儿加护病房里住了几天,花费医疗系统大量资源。所有这些没有必要的过程都是因为医院“例行”对血糖进行检测。这个宝宝并没有低血糖的风险因子。
If you need help with breastfeeding, make an appointment at our clinic.
如需母乳喂养方面的帮助,可以向我们的诊所预约。
