Jaundice, a yellow coloration of the skin, is due to a rise in the blood of bilirubin, a yellow pigment that comes from the breakdown of old red blood cells. Red blood cells do not live forever, and thus it normal for old red blood cells to break down, but the bilirubin formed does not usually cause jaundice because the liver metabolizes it and gets rid of it into the gut. The newborn baby, however, often becomes jaundiced during the first few days because the liver enzyme that metabolizes bilirubin is relatively immature. Furthermore, newborn babies have more red blood cells than adults, and thus more are breaking down at any one time; as well many of these cells are different from adult red cells and they don’t live as long. All of this means more bilirubin will be made in the newborn baby’s body and less will be broken down. If the baby is premature, or stressed from a difficult birth, or the infant of a diabetic birth parent, or more than the usual number of red blood cells are breaking down (as can happen in blood incompatibility), the level of bilirubin in the blood may rise higher than usual levels. See also our blog Breastfeeding, Bilirubin and Jaundice
It should be emphasized that bilirubin has an undeserved bad reputation. It is more like an innocent bystander that is blamed for brain damage when in fact, the problem is not the bilirubin, which plays only a minor part in the process. It is the set of circumstances that allowed the bilirubin to enter the brain that is the real problem. Severe lack of oxygen when the baby is asphyxiated or severe anemia due to very rapid breakdown of red blood cells, Rh incompatibility or ABO incompatibility, which is also associated with metabolic disturbances causes the damage to the blood-brain barrier that allows bilirubin to enter the brain and made physicians believe that the bilirubin was the basic problem. In fact, bilirubin is an antioxidant and actually protects the baby from damage.
The most common cause of higher than average bilirubin levels in the first few days of life is not breastmilk, but rather the fact that the baby is not breastfeeding well and not getting adequate amounts of breastmilk. Though giving formula works to bring down the bilirubin, giving formula, especially by bottle, interferes with breastfeeding as bottles teach the baby a poor latch, which then cause the mother sore nipples and/or result in the baby not getting enough milk from the breast. The answer is for the mother to get good help with breastfeeding and only if the baby still does not get adequate amounts of milk from the breast, then supplementation should be considered and given by lactation aid at the breast.
For even more information about jaundice, click here.
TWO TYPES OF JAUNDICE
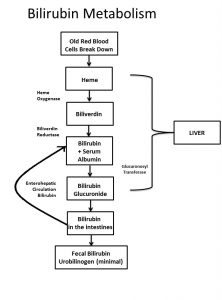
The liver changes bilirubin so that it can be eliminated from the body (the changed bilirubin is now called conjugated, direct reacting, or water soluble bilirubin–all three terms meaning essentially the same thing). If, however, the liver is functioning poorly, as occurs during some infections, or the tubes that transport the bilirubin to the intestines are blocked, this changed bilirubin may accumulate in the blood and also cause jaundice. When this occurs, the changed bilirubin appears in the urine and turns the urine brown or brownish. This brown urine is an important clue that the jaundice is not “ordinary”. Jaundice due to conjugated bilirubin is always abnormal, frequently serious and even life-threatening, and needs to be investigated thoroughly and immediately. Except in the case of a few extremely rare metabolic diseases, breastfeeding can and should continue.
Accumulation of bilirubin before it has been changed by the enzyme of the liver may be normal— “physiologic jaundice” (this bilirubin is called unconjugated, indirect reacting or fat soluble bilirubin). Physiologic jaundice begins about the second day of the baby’s life, peaks on the third or fourth day and then becomes unnoticeable on the baby’s skin. However, there may be other conditions that may require treatment that can cause an exaggeration of this type of jaundice. Because these conditions have no association with breastfeeding, breastfeeding should continue. If, for example, the baby has severe jaundice due to rapid breakdown of red blood cells, this is not a reason to take the baby off the breast. Breastfeeding should continue in such a circumstance.
SO-CALLED BREASTMILK JAUNDICE
There is a “condition” commonly called breastmilk jaundice. No one knows what the cause of breastmilk jaundice is. In order to make this diagnosis, the baby should be at least a week old, though interestingly, many of the babies with breastmilk jaundice also have had exaggerated physiologic jaundice. The baby should be gaining well, breastfeeding exclusively, having lots of bowel movements, passing plentiful, clear urine and be generally well (see the information sheet “Is my Baby Getting Enough Milk?” and our video clips showing how to tell if the baby is drinking well or not). In such a setting, the baby has what some call breastmilk jaundice, though, on occasion, infections of the urine or an under functioning of the baby’s thyroid gland, as well as a few other even rarer illnesses may cause the same picture. Breastmilk jaundice peaks at 10-21 days, but may last for two or three months. Breastmilk jaundice is normal. Rarely, if ever, does breastfeeding need to be discontinued even for a short time. Only very occasionally is any treatment, such as phototherapy, necessary. Yes, interrupting breastfeeding for a day or two will bring down the bilirubin, but a day or two of bottle feeding may result in breastfeeding becoming very difficult. Some babies have refused to latch on after 24 to 48 hours of bottle feeding.
There is not one bit of evidence that this type of jaundice causes any problem at all for the baby. Breastfeeding should not be discontinued “in order to make a diagnosis”. If the baby is truly doing well on breast only, there is no reason, none, to stop breastfeeding or supplement even if the supplementation is given with a lactation aid, for that matter. The notion that there is something wrong with the baby being jaundiced comes from the fact that the formula feeding baby is the model we think is the one that describes normal and we impose this abnormal “normal” on the breastfed baby. This manner of thinking, almost universal amongst health professionals, truly turns logic upside down. Thus, the formula feeding baby is rarely jaundiced after the first week of life, and when he is, there is often something wrong. Therefore, the baby with so called breastmilk jaundice is a concern and “something must be done”. However, in our experience, most exclusively breastfed babies who are perfectly healthy and gaining weight well are still jaundiced at five to six weeks of life and even, not uncommonly to 3 or 4 months of age. The question, in fact, should be whether or not it is normal not to be jaundiced and is this absence of jaundice something we should worry about?
Do not stop breastfeeding for “breastmilk” jaundice. “Breastmilk jaundice” does not need to be treated. It is normal!
NOT-ENOUGH-BREASTMILK JAUNDICE
Higher than usual levels of bilirubin or longer than usual jaundice may occur because the baby is not getting enough milk. This may be due to the fact that the mother’s milk takes longer than average to “come in” (but if the baby feeds well in the first few days this should not be a problem), or because hospital routines limit breastfeeding or because, most likely, the baby is poorly latched on and thus not getting the milk which is available (see the information sheet “Is my Baby Getting Enough Milk?” and our video clips showing how to tell if the baby is drinking well, or not). When the baby is getting little milk, bowel movements tend to be scanty and infrequent so that some of the bilirubin that was in the baby’s gut gets reabsorbed into the blood instead of leaving the body with the bowel movements. Obviously, the best way to avoid “not-enough-breastmilk jaundice” is to get breastfeeding started properly (see the information sheet “Breastfeeding—Starting Out Right”). Definitely, however, the first approach to not-enough-breastmilk jaundice is not to take the baby off the breast or to give bottles, which are likely to make the breastfeeding work even less well. If the baby is breastfeeding well, more frequent feedings may be enough to bring the bilirubin down more quickly, though, in fact, nothing really needs be done for breastmilk jaundice except to reassure the parents.
If the baby is breastfeeding poorly, helping the baby latch on better may allow him to breastfeed more effectively and thus receive more milk. Compressing the breast to get more milk into the baby may help (see the information sheets “Latching and Feeding Management” and “Breast Compression”). If latching and breast compression alone do not work, a lactation aid would be appropriate to supplement feedings (see the information sheet “Lactation Aid”). See also the information sheet “Protocol to Increase Breastmilk Intake” and our video clips for help with latching, how to know the baby is getting milk, how to use compressions, as well as other information.
PHOTOTHERAPY (BILIRUBIN LIGHTS)
Phototherapy increases the fluid requirements of the baby. If the baby is breastfeeding well, more frequent feeding can usually make up this increased requirement. However, if it is felt that the baby needs more fluids, use a lactation aid to supplement, preferably expressed breastmilk, expressed milk with sugar water or sugar water alone rather than formula.
However, to emphasize again, if the baby is breastfeeding well, drinking well at the breast, gaining weight well, there is no need for bilirubin lights to treat the jaundice.
The information presented here is general and not a substitute for personalized treatment from an International Board Certified Lactation Consultant (IBCLC) or other qualified medical professionals.
This information sheet may be copied and distributed without further permission on the condition that you credit International Breastfeeding Centre and it is not used in any context that violates the WHO International Code on the Marketing of Breastmilk Substitutes (1981) and subsequent World Health Assembly resolutions. If you don’t know what this means, please email us to ask!
©IBC, updated July 2009, June 2017, 2021
Questions or concerns? Email Dr. Jack Newman (read the page carefully, and answer the listed questions).

